Due to the recent COVID19 pandemic there are many wondering about how cannabinoids affect the immune system. Do hemp products assist or weaken the body’s ability to fight off a viral infection? Although scientific studies are few, there are indications that cannabidiol (CBD) may selectively suppress the immune system leaving the immune system viral-fighting ability intact. The question of whether cannabis or hemp products assist or hurt the body’s ability to fight a viral infection is complicated and to be honest, not straightforward, due to the intricacy of the immune system and the number of components in full spectrum hemp or marijuana products. To understand how cannabidiol may be a potential supplement to help the immune system, it is first necessary to have a basic understanding of the immune system, describe the Endocannabinoid System (ECS) and the components in hemp oil, then summarize studies describing describe how cannabidiol influences the immune system. Overall, the research suggests that THC suppresses the immune system and may hinder the ability to combat a viral infection, whereas the data is insufficient to conclude whether CBD helps an immune response. Instead, CBD may be a beneficial supplement to combat secondary infection through its reported anti-bacterial properties and to ease aches and pains associated with a viral infection.
How does our immune system combat infection?
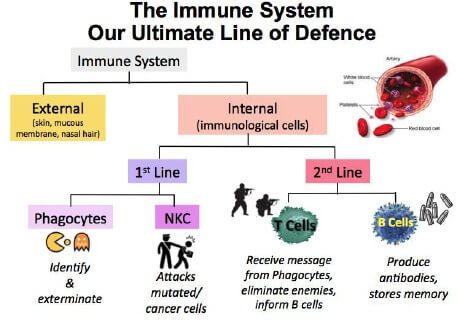
Figure 1 shows a simplified description of the human immune system. The immune system is very complex consisting of several organs and cell types which are needed to fight off a variety of infectious agents including viruses, bacteria, molds and parasites and can be reviewed in more detail here. The first line of defense is to form a physical barrier to the invading organism provided by our skin and mucous membranes located in the nose, mouth, and eyes. If a virus, for example enters through a nick in the skin, or penetrates mucous membranes then the second line of defense is activated to identify, isolate and eliminate the invader. The immune system also has a mechanism to remember the invader so a more rapid response can be mounted for future infections.
In simplistic terms the immune system can be divided into two categories: The innate and adaptive immune systems. Both systems have intricate mechanisms to determine self from non-self so that the immune response is mounted only against foreign invaders. Innate immunity is present from the time of birth and is a non-specific defense consisting of multiple types of white blood cells. These cells identify the infective agent and causes an inflammatory cascade to bring more infection fighting cells to the site of injury. The inflammatory reaction attempts to isolate the injury as much as possible trying to eliminate the foreign invader before an active infection is started. When the white blood cells destroy the infective organism they will display antigens (pieces of the foreign invader that can be used for future recognition) for an adaptive immune response. In some cases, the innate immune response is not enough to combat the foreign body or the pathogen is able to exploit the immune response by hiding in host cells, such as viruses. In such situations the innate immune system works with the adaptive immune system to reduce severity of infection while fighting off any additional invaders.

The adaptive immune system mounts a response specific to the invading pathogen taking a bit longer to respond to new organisms. Adaptive immunity consists of multiple types of B and T cells. B cells produce antibodies specific to the foreign organism called humoral immunity. Antibodies will bind to foreign bodies such as bacteria and target them for elimination and destruction. For viruses that invade normal cells, cell-mediated adaptive responses are needed which is where T-cells are important. T-cells need to be able to distinguish between self and non-self to ensure only cells infected with parasites or viruses are destroyed. Although there are multiple types of T-cells, they can be divided into three main groups: T helper cells (CD4), Cytotoxic T cells (CD8) and regulatory T cells (CD8/CD25). T helper cells activate B cells, cytotoxic T cells and other immune cells. Cytotoxic T cells, CD8 cells are responsible for removing pathogens and infected host cells. Regulatory T cells assist in distinguishing between self and non-self to reduce the risk of autoimmune diseases.
Figure1. Immune System Overview
The Endocannabinoid System (ECS)
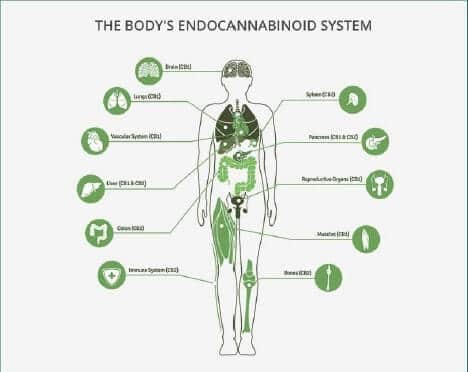
The ECS is a system of receptors and enzymes located throughout the body exerting a broad range of effects as shown in Figure 2. Discovered in the late 1980s, the ECS was first thought to be comprised only of the Cannabinoid 1 (CB1) and cannabinoid 2 (CB2) receptors. This definition has evolved to include as many as 50 receptors and enzymes that interact with various cannabinoids. The large and varied number of targets cannabinoids interact with explains the number of conditions or biological processes the ECS influences.

-

CBD + CBG Body Massage Oil
From: $9.95 Select options This product has multiple variants. The options may be chosen on the product page -

Cannabidiol Oral Solution
$36.95 Add to cart -

CBD Softgels for Sleep 50mg
$37.45 Add to cart
Our bodies produce endogenous cannabinoids, termed endocannabinoids, that regulated the ECS. Two identified cannabinoids, Anandamide (Correct name AEA), and 2-arachidonyl Glycerol (2-AG), are produced in the body to help maintain correct body function. Both of these endocannabinoids have overlapping yet distinct functions that influence the immune system as well as other actions.
While there is much to be learned about the ECS, the system appears to function as a regulator of various physiological functions to return the body back into balance, or to normalize biological responses termed homeostasis. In the case of the immune system, the ECS dampens the inflammatory response to lessen the possibility of dysregulation.
Figure 2. Endocannabinoid System CB1 and CB2 Receptor Distribution.
Cannabinoids and the immune system.
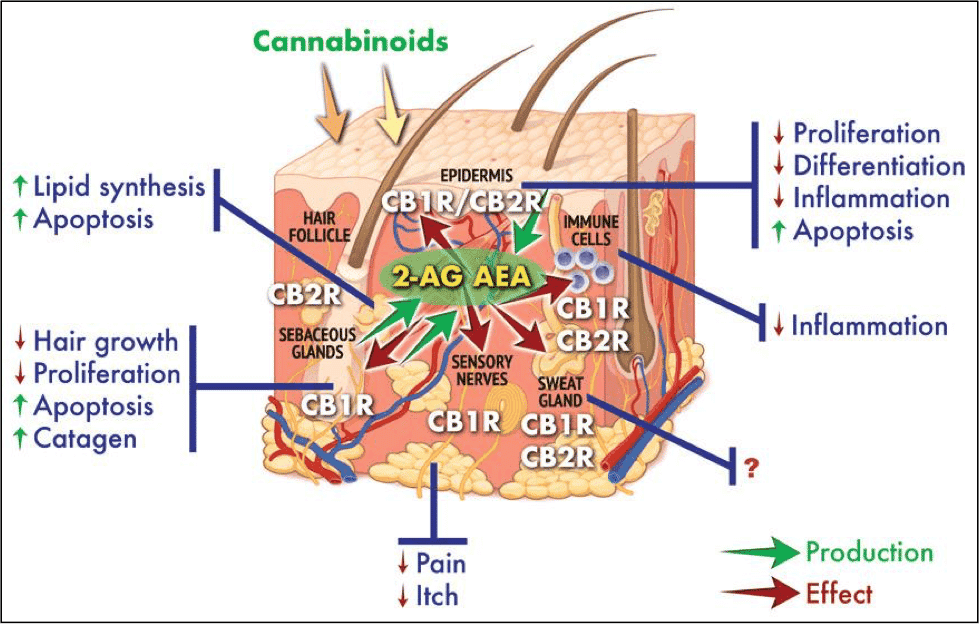
As stated earlier, there are a small number of studies published on the effects of cannabinoids on the immune system with those that have been published not providing a clear picture of action. Cannabinoids appear to affect the immune system primarily through the CB2 receptor. This receptor is expressed on multiple immune cells and when activated by cannabinoids decrease overall inflammation eliciting a shift in cytokine expression (secreted proteins that signal amongst immune cells) from a Th1-pro inflammatory type to a Th2 anti-inflammatory profile (Th is a designation for a T helper cell). While studies consistently conclude that cannabinoids and activity at the CB2 receptor suppress inflammation and immune function, there appear to be differential activities amongst both endogenous (e.g. Anandamide or 2-acrachidonoylglycerol) and phytocannabinoids on the immune system overall.
Anandamide (AEA) affects cellular communication amongst immune cells by lowering the expression of several immune proteins. Whereas AEA exhibits an inhibitory effect on immune function, 2-acrachidonoylglycerol (2-AG) augments immune function by increasing the release of nitric oxide (used to destroy target cells) and to increase immune cell motility through both CB1 and CB2 related mechanisms. The differential responses by these cannabinoids are most likely mediated through receptors and/or enzymes distinct from CB2 that have not been fully described as of yet.
Similarly, THC and CBD exert overlapping yet distinct effect on the immune system. Much of the information regarding THC stems from studies in human immunodeficiency virus infected patients or models. Overall, THC suppresses the immune system but some of the results are conflicting. In HIV patients, CB2 activation by THC has been reported to reduce morbidity and has favorable effects on gut mucosal immunity, decrease CD4 T-Cell infection rates, reduce lymph node fibrosis and diminishes viral counts. A 2015 study showed that patients who ingested cannabis had much lower viral loads from patients who did not use it and HIC patients participating in this study had higher CD4 cell numbers. Another study showed a 20% increase in the number of CD4 and CD8 cells compared to those who didn’t.
In contrast, it has been demonstrated that cannabinoids decreased host resistance to a variety of infectious agents. Administration of THC to mice lessened their ability to resist infection of listeria monocytogenes and herpes simplex virus 2. THC also increased the incidence of viral lesions and recurrences of genital herpes. THC has also been reported to suppress proliferation of B and T lymphocytes in response to specific mitogens and suppress cytolytic activity of Natural Killer cells. The collective data suggests that THC inhibits the functional activities of a variety of immunological cells and that the outcome is consistent with decreasing host resistance to infectious agents which may enhance disease progression and lead to death in the worst case.
Like THC, there are few studies on the effects of CBD on the ability to boost the immune system to combat viral infections. In a study focused on viral hepatitis the role of CBD in hepatitis B and hepatitis C viral infections were evaluated. CBD was successful in limiting the replication of the Hep C virus but had no effect on hep B. CBD reduced HCV replication in a concentration-dependent manner by up to 86%. CBD also reduced Karposi’s sarcoma associated virus proliferation and enhanced apoptosis (programmed cell death) of infected cells at low concentrations that are easily achieved in humans in a well-tolerated therapeutic dose. Note that THC may enhance infection and replication of KSHV and promote KSHV endothelial transformation. The proposed mechanism for inhibition of these viruses was through activation of the adenosine A2A receptor.
However promising these results may be, scientific data does not conclusively demonstrate whether cannabinoids are effective at boosting the immune system to help combat viral infections. If anything, THC may increase risk for infection and has been shown to be a risk factor for Mycobacterium tuberculosis (TB) infection. Any claims regarding the use of cannabis or industrial hemp products to combat viral infection by cannabis manufacturers is false and misleading.
Where cannabidiol can help: secondary infection ease of aches and pains
Viral respiratory tract infections (VRTIs) are very common with presentations varying from simple colds to life-threatening infections. In the course of a viral infection, the virus debilitates the mucociliary clearance structure which leads to the increased attachment of bacteria to mucins and colonization occurs. The mucus build-up impedes the penetration of antibacterial material and immune cells. Bacterial coinfection occurs in up to 60% of VRTIs. In the 1918 flu epidemic it was estimated that of the 50 million deaths many were due to secondary bacterial pneumonia with Streptococcus pneumoniae.
At the 2019 American Society for Microbiology Microbe, Dr. Mark Blaskovich reported that cannabidiol possessed gram positive antimicrobial activity with potencies similar to antibiotics vancomycin and daptomycin. The report also stated that cannabidiol did not lose effectiveness with repeated applications as seen with other antibiotics and had the ability to dissolve biofilms produced by gram positive bacteria. A subsequent study at the University of Southern Denmark demonstrated that Cannabidiol is an effective “helper” compound that when used in combination with bacitracin, an antibiotic, potentiated bacitracin effects on killing gram positive bacteria including antibiotic resistant bacteria.
Although clinical studies should be conducted, these findings suggest that CBD may be effective at preventing or treating gram positive secondary infections subsequent to VRTIs. Additionally, inclusion of CBD in soaps for surface or hand cleaning may help lower the incidence of infection by gram positive bacterial such as staphylococcus species in settings where these bacteria are prevalent, such as hospitals.
Concluding remarks:
Scientific evidence regarding CBD effects to stimulate the immune system’s ability to combat viral infection is disparate and inconclusive. Specific studies need to be conducted to determine whether CBD is effective at helping immune cells resist or minimize infection to influenza or cold viruses. In many cases, cannabinoids may exacerbate the condition, especially if dosed by inhalation. The true value of CBD for those ailing from a viral infection will be to ease the aches and pains, such as a sore throat, caused by the viral infection, and to protect/combat secondary bacterial infections